Precision Medicine
- Surviving Breast Cancer

- Aug 7, 2022
- 4 min read
Updated: Oct 30, 2025

Precision medicine, according to the National Research Council, focuses “on identifying which approaches will be effective for which patients based on genetic, environmental, and lifestyle factors.” Once doctors have this important information regarding your tumor and genetics, they can make informed recommendations related to your diagnosis and treatment plan.
A breast cancer diagnosis unites us, and it provides a common thread as we share stories about treatments, surgeries, and coping mechanisms. Within breast cancer circles, however, we quickly jump to questions about one’s HER2 status, hormone receptor status, or whether or not we opted for genetic testing. We have the ability to rattle off pharmaceutical and generic name drugs, which aromatase inhibitor we are on, and the bond we innately forge when we meet someone else who is also Triple Negative, or BRCA Positive.
(Watch the Webinar)
We have these conversations with our breast cancer besties, and we start to identify our “breast cancer twin”. That is to say, someone else diagnosed around the same age, with the same stage and type of breast cancer.
However, if we have found our breast cancer twin, then why do we have different side effects? Why would my cancer twin have a complete response to neo-adjuvant chemotherapy (receiving chemotherapy prior to surgery), whereas I did not? Why did my cancer come back (recurrence) 4 years later, and hers did not?
How Precision Medicine Provides Answers
Precision medicine enables us to answer some of these tough questions and to identify specific treatment options based on our tumor characteristics. For example, if you have tested positive for the HER2 gene, oncologists recognize that this particular gene causes the cancer to grow and spread faster than if you tested negative for HER2. If you do have HER2+ breast cancer, the good news is that there are targeted therapies, such as Herceptin, that work to slow or even stop the growth of the cancer cells by blocking any signals trying to get to the HER2 protein. Because of precision medicine, researchers have been able to develop targeted therapies to benefit those diagnosed with HER2+ breast cancer.
Precision medicine can improve disease detection and preempt disease progression. It also places emphasis on prevention rather than just serving as a reaction to a particular disease. Concisely, precision medicine is an attractive option as it can help us to better understand cancer, Alzheimer’s, diabetes, and many other illnesses that plague us.
DNA is the Key to Advancement
Technological advances have enabled researchers and scientists to decode DNA at lightning speed. If we can decode our genes, understand what secrets they hold, and harness that information to target, treat, and prevent disease, we are literally holding the golden ticket. In 2015, under then-President Barack Obama, the National Institute of Health (NIH) launched a national, patient-powered research initiative seeking one million or more Americans to volunteer as participants in research.
In order to understand the human genome and the onset of disease, scientists and researchers will need a substantial and very diverse sample size. This is a heroic opportunity for people to get involved in the advancement of medicine. However, it is easier said than done.
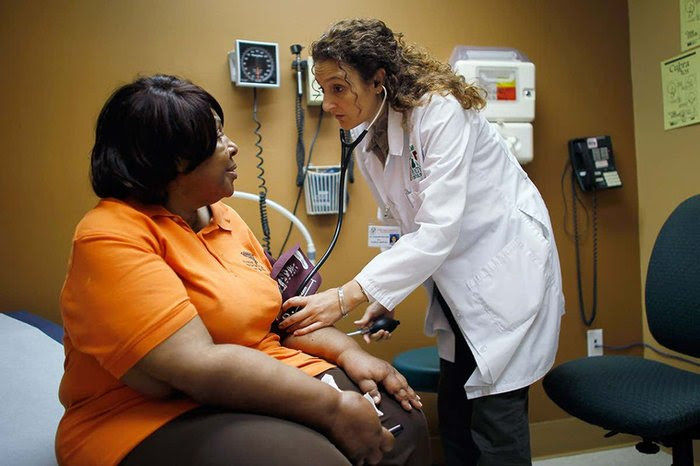
There is currently a lack of trust in Science and Medicine. Smirnoff, Willets, and their team (2018) identified a framework for understanding specific areas of research trust/mistrust amongst disparate study populations. In their published paper, A paradigm for understanding trust and mistrust in Medical Research: The Community VOICES Study, the scholars laid out four pillars that offer a conceptual framework in order to strengthen truths and increase broader participation in clinical research. The areas are:
General Trustworthiness (Older age, not disabled)
Perceptions of Discrimination (African American, Latino, Spanish Language Preference)
Perceptions of Deception (prior research experience, African American)
Perceptions of Exploitation (less education)
Despite federal mandates to ensure the inclusion of women and minorities in federally funded research, there continues to be additional barriers to participation, including “logistical problems, low levels of health literacy, and sociocultural factors” (Scharff, Mathews, Jackson, Hoffsuemmer, Martin & Edwards, 2010).
Issues with Past Studies
If we take a look at the Tuskegee Study, why wouldn’t one be skeptical? The Tuskegee Study was a 40-year experiment run by Public Health Service Offices who followed 600 rural black men in Alabama with syphilis over the course of their lives, refusing to tell them of their diagnosis, refusing to treat them, and denying them treatment.
The U.S. has a long-rooted history ingrained in our system and structures, but we need to overcome this. We can do better. As a result of the horrific experiment of the Tuskegee Study, policies and legislation were formed to protect human subjects. For example, researchers need to obtain voluntary informed consent and have their research reviewed and approved by institutional review boards to ensure that ethical standards are met.
To begin, we need to recognize that precision medicine does have its perils. While we’ve been focusing on the advantages, such as unlocking the information hidden within our DNA, we as a society need to do better to ensure we are including all of the players and inviting them to the table.
There are ethical considerations that must be explored before we hand over our genetic information for research. For example, what are the legal ramifications of sharing your DNA? Who owns the data? Can an employer or life insurance company discriminate against you based on your genetic information?
How can we get it right? We have an opportunity to rebuild trust, to improve clinical trial participation, and to support research; this initiative is bigger than any individual, it is the sum of one million data points to ensure that our sons, daughters, and their children have access to the best medicine and preventative care in years to come.
References:
Smirnoff, M., Wilets, I., Ragin, D. F., Adams, R., Holohan, J., Rhodes, R., Winkel, G., Ricci, E. M., Clesca, C., & Richardson, L. D. (2018). A paradigm for understanding trust and mistrust in medical research: The Community VOICES study. AJOB empirical bioethics, 9(1), 39–47. https://doi.org/10.1080/23294515.2018.1432718
Scharff, D. P., Mathews, K. J., Jackson, P., Hoffsuemmer, J., Martin, E., & Edwards, D. (2010). More than Tuskegee: understanding mistrust about research participation. Journal of health care for the poor and underserved, 21(3), 879–897. https://doi.org/10.1353/hpu.0.0323











